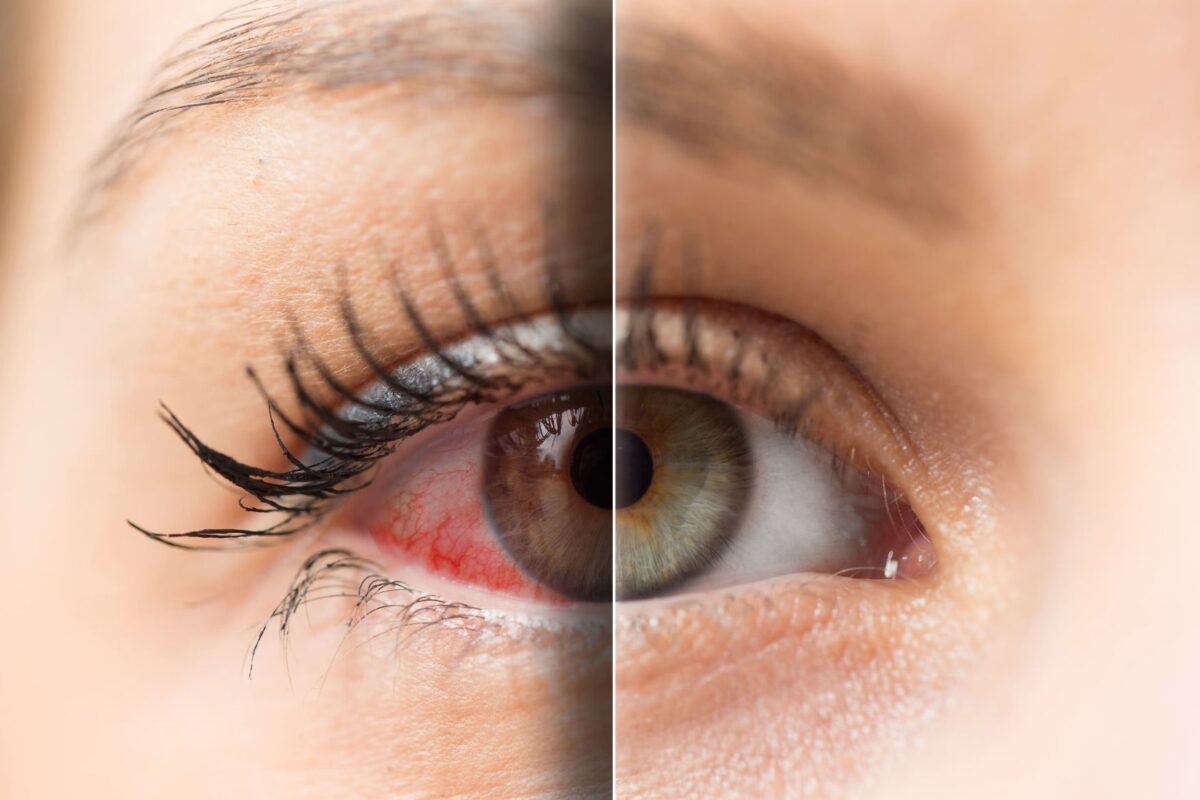
Regenerative medicine focuses on repairing damaged tissue and regenerating missing or lost tissue while restoring normal form and function. Regenerative medicine works by stimulating your body’s own natural ability to repair and regenerate itself.
Exosome Therapy
Exosome therapy for the treatment of dry eye disease.
Meibomian gland dysfunction, blepharitis, ocular rosacea and allergic conjunctivitis (collectively known as ocular surface disease, OSD) is an exciting and innovative approach which works by reducing inflammation, repairing damaged tissue and regenerating lost tissue. While exosome therapy is still undergoing research and clinical trials, it has shown great potential and promise as an effective treatment for patients who suffer from ocular surface diseases, especially when first line, conventional treatments haven’t provided sufficient relief.
In clinical practice the work with exosomes is derived from umbilical cord stem cells formulated as an extract which is instilled as eye drops. These drops are filled with growth hormones, anti-inflammatory cytokines, amino acids, proteins, lipids, and exosomes which stimulate the body’s own natural ability to heal, repair, regrow and regenerate cells and tissue. This extract is biologically active with the ability to differentiate into any cell or tissue type it contacts because it’s derived from pluripotent embryonic stem cells.
In dry eye disease, Meibomian gland dysfunction, blepharitis, ocular rosacea and allergic conjunctivitis (OSD), the corneal and conjunctival epithelial cells, and the lacrimal and Meibomian glands, are damaged due to chronic dryness and inflammation. Exosome therapy reduces inflammation supporting the healing, repair and regeneration of the ocular surface, and the lacrimal and Meibomian glands, thus improving the overall health and comfort of the eyes and eyelids.
Two key factors involved in dry eye disease, Meibomian gland dysfunction, blepharitis, and ocular rosacea are insufficient tear production by the lacrimal glands and insufficient oil production by the Meibomian glands. Exosome therapy can help stimulate the repair and regeneration of the lacrimal and Meibomian glands in both form and function. This results in the production of better quality and quantity of tears by the lacrimal glands and oil by the Meibomian glands, thus stabilizing the tear film, increasing comfort, and enhancing vision by supporting a smoother, healthier ocular surface.
Autologous Serum
Autologous Serum drops are used in the treatment of dry eye disease, Meibomian gland dysfunction, blepharitis, ocular rosacea and allergic conjunctivitis (OSD). They lubricate and promote healing and repair of the surface of the eyes, the lacrimal and Meibomian glands, and the eyelids. Autologous serum is custom made eye drops which take advantage of your own body’s natural growth factors, immunoglobulins, anti-inflammatory cytokines, antibodies, vitamins and other essential components in your blood. Dr. Muller arranges for you to have your blood drawn (as if you were donating blood), your blood is spun down using a centrifuge, and the serum is made into eye drops. Autologous serum drops have been shown to increase the health and comfort of the eyes and eyelids, decrease inflammation and scarring, promote healing and repair, enhance vision by supporting a smoother, healthier ocular surface, and make patients much more comfortable by reducing symptoms such as dryness, irritation, and redness.
Amniotic Membranes
Amniotic membranes are another innovative treatment used to enhance and facilitate healing and reduce inflammation for the treatment of dry eye disease, Meibomian gland dysfunction, blepharitis, ocular rosacea, allergic conjunctivitis, and other ocular conditions.
Amniotic membranes are therapeutic biologic corneal bandages (similar to contact lenses). These corneal bandage lenses are composed of amniotic membrane derived from the innermost layer of placental tissue which contains growth factors, anti-inflammatory cytokines, and extracellular matrix proteins that promote healing and repair of damaged tissue, and reduce inflammation. The natural therapeutic properties of these membranes also help decrease the risk of complications such as corneal ulcers or infections, mitigate scarring, enhance comfort, and improve vision by creating a smoother, healthier ocular surface.
A consultation with Eye Specialist is necessary to determine if these new modalities and latest treatment approaches are viable cure options for your specific eye problem related to Ocular Surface Disease.